Metabolic Modeling Predicts Unique Drug Targets in Lyme Disease Pathogen B. burgdorferi – TUSM’s Peter Gwynne, PhD
February 23, 2023
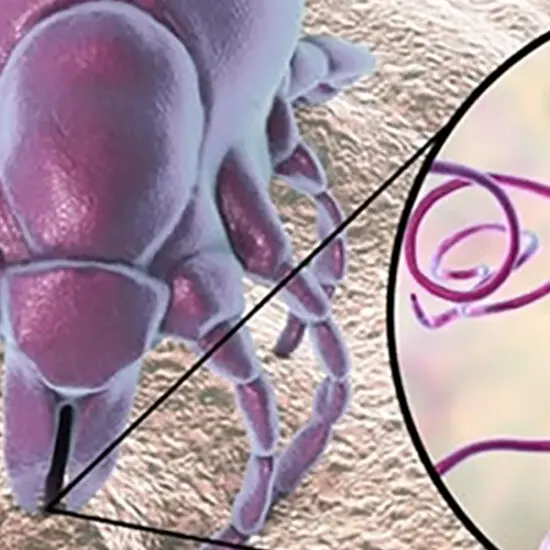
We were pleased to hear from Bryan Lenneman, Ph.D., today on “Engineering Phages as Novel Antimicrobials Targeting Gram-Negative Pathogens.” Dr. Lenneman is a Research Fellow at Massachusetts General Hospital whose research interests include utilizing synthetic biology to develop novel therapeutics against diseases associated with dysbiosis of the human gut microbial community.
Engineering Phages as Novel Antimicrobials Targeting Gram-Negative Pathogens – Massachusetts General Hospital’s Bryan Lenneman, Ph.D.
March 30, 2023
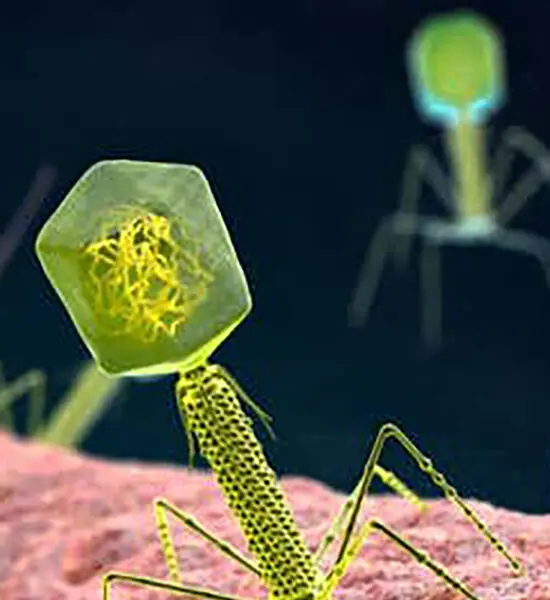
MGH Research Fellow Bryan Lenneman, PhD, is interested in utilizing synthetic biology to develop novel therapeutics against diseases associated with dysbiosis of the human gut microbial community.
CIMAR Joins the Battle Against AMR with Collaborative and Brainstorming Workshop
January 21, 2019

The Tufts Center for Integrated Management of Antimicrobial Resistance (CIMAR) hosted its first event last month to introduce the Center to the local scientific community and to offer a platform for investigators and clinicians to showcase their research and promote collaborations. CIMAR aims to address the rise and spread of antimicrobial resistance (AMR), and we believe our faculty possess the myriad unique skillsets needed to lead this fight. Roughly 700,000 human deaths are attributable to AMR each year globally, and if trends continue, AMR could contribute to a total of 350 million deaths by 2050.
Exploring The Intersection Of Racism, Antimicrobial Resistance, And Vaccine Equity — UC San Diego’s Jacinda C. Abdul-Mutakabbir PharmD, MPH, AAHIVP
February 29, 2024

Dr. Jacinda Abdul-Mutakabbir explores the intersection of antibiotic resistance and health/vaccine equity, with a specific focus on racial differences observed across racially and ethnically minoritized groups.
You and Your Pet Can Share Resistance to Certain Medications. Here’s How.

People are in such close contact with their dogs, cats, and other pets that research shows they often share flora, or tiny bacteria and other microorganisms that inhabit the skin, gut, and even the environment of the home. If you or your pet take an antibiotic or another antimicrobial medication, it can potentially change the flora you both carry. And if your pet is carrying antimicrobial resistant bacteria, which may lessen the efficacy of prescribed medications, you may be, too. Small-animal veterinarians at the Tufts Cummings School of Veterinary Medicine are leading nationwide efforts to understand antimicrobial stewardship and resistance in companion animals.
How the Pandemic Gave Power to Superbugs: Tufts Dean Weighs In
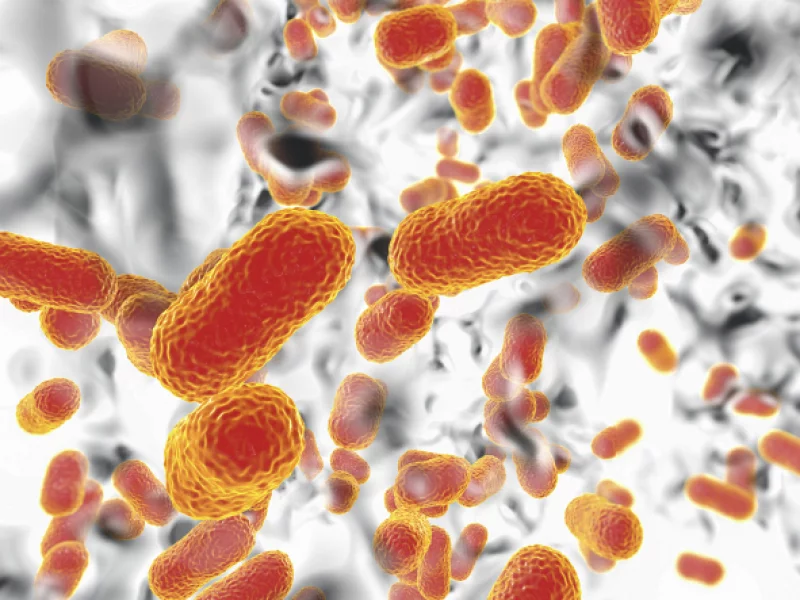
Antibiotics cannot cure COVID. They don’t help a bit. And yet, new data shows that, during the pandemic, COVID patients were given antibiotics – a lot of antibiotics. That’s bad because the overuse of antibiotics can breed superbugs that are resistant to medications. The impact of this pandemic overuse has lingered even as the pandemic has faded. So how did this unfortunate turn of events come to be? A series of new reports and papers shed light. Globally, about 75% of patients hospitalized with COVID were given antibiotics, despite only 8% having a bacterial coinfection where antibiotics would be medically useful. This comes from new data published in late April that was collected through the World Health Organization’s Global Clinical Platform in 65 countries between January 2020 and March 2023.
Levy CIMAR's New Research Hub to Tackle Antimicrobial Resistance

n a significant stride toward combating the global threat of antimicrobial resistance, Tufts University has launched the Laboratory for Combinatorial Drug Regimen Design for Resistant and Emerging Pathogens (LCDRD). Made possible by a $5.15 million grant from the National Institutes of Health, the new facility is housed within the Levy CIMAR and located on the 8th floor of Tufts’ Biomedical Research and Public Health Building on its Health Sciences Campus in Boston. The 2,500-square-foot lab is designed to foster collaboration among scientists, clinicians, and engineers from across Tufts University, Tufts Medicine, and national and international partners. Situated adjacent to Tufts’ BSL-3 lab and key research groups, it supports a uniquely interdisciplinary research environment with state-of-the-art investigative and safety amenities.
- Metabolic Modeling Predicts Unique Drug Targets in Lyme Disease Pathogen B. burgdorferi – TUSM’s Peter Gwynne, PhDFebruary 23, 2023
- Engineering Phages as Novel Antimicrobials Targeting Gram-Negative Pathogens – Massachusetts General Hospital’s Bryan Lenneman, Ph.D.March 30, 2023
- CIMAR Joins the Battle Against AMR with Collaborative and Brainstorming WorkshopJanuary 21, 2019
- Exploring The Intersection Of Racism, Antimicrobial Resistance, And Vaccine Equity — UC San Diego’s Jacinda C. Abdul-Mutakabbir PharmD, MPH, AAHIVPFebruary 29, 2024
- You and Your Pet Can Share Resistance to Certain Medications. Here’s How.

